U.S. Antibiotic Awareness Week is November 13-19, 2017 and is intended to raise awareness of the threat of antibiotic resistance and the importance of appropriate antibiotic prescribing and use.
Since the 1940s, antibiotics have transformed our ability to treat infections effectively. Unfortunately inappropriate antibiotic use has led to increasing antibiotic resistance. Now these lifesaving drugs do not work as well as they once did, and successfully treating common infections has become more difficult.
Every year in the United States, more than 2 million people become infected with bacteria that are resistant to antibiotics and at least 23,000 people die as a direct result of these infections. Many more people die and have serious health consequences from antibiotic-resistant infections and antibiotic side-effects.
How do antibiotics create resistant bacteria?
- Every time a person takes an antibiotic, sensitive bacteria are killed, but resistant ones may be left to grow and multiply. These resistant bacteria can then cause hard to treat infections and spread to other people.
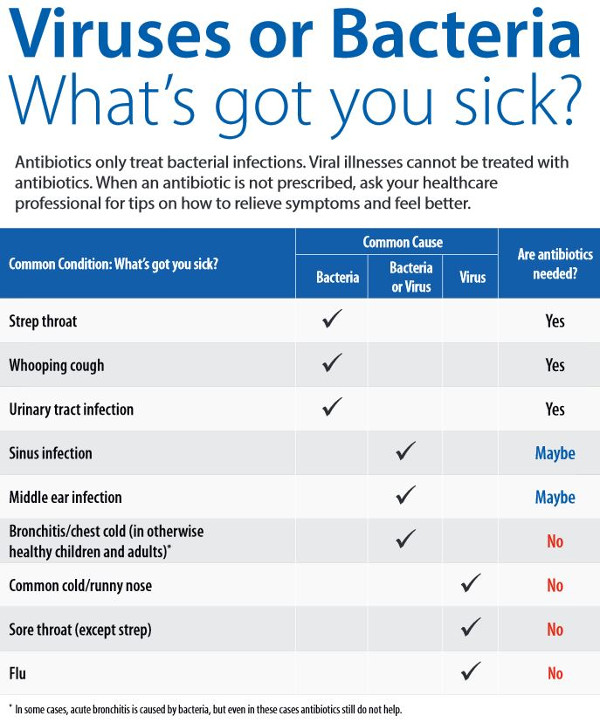
As we enter the winter when respiratory infections are more common, it is important to know what types of infections need antibiotics and what type of infections do not. Taking antibiotics for some types of infections can put you at risk without providing any benefit.
Check out the chart below from the Centers for Disease Control and Prevention (CDC) to learn about which infections need antibiotics and which do not. Dr. Perales and Dr. Donesa-Zuzak aim to:
- Use antibiotics only when they are needed so they will work for you when you need them and will not cause harm when you don't need them.
- Help you with symptom relief from infections so you feel better as soon as possible.
Take the CDC's Antibiotics Quiz to test your knowledge about antibiotics and antibiotic resistance.
Learn more about what you and your family can do to use antibiotics safely and appropriately:
- CDC - What You Can Do
- ReAct - What Can I do?
- TED talk about the coming antibiotic resistance crisis by Ramanan Laxminarayan Senior Research Scholar and Lecturer at Princeton University
- Arizona Department of Health Services - FAQ